Emphysema: Overview
Emphysema is a chronic pulmonary condition with loss of elasticity in the alveoli and the interalveolar septa – the "meat-foam" and their interleaving sheaths that fill up when we breathe. Lung tissue that exchanges oxygen and carbon dioxide is destroyed, causing shortness of breath.
- check your overall health status
- understand what's happening to your body
- learn what you should be doing right now
Emphysema is considered to be a type of Chronic Obstructive Pulmonary Disease (COPD) and usually occurs alongside Chronic Bronchitis.
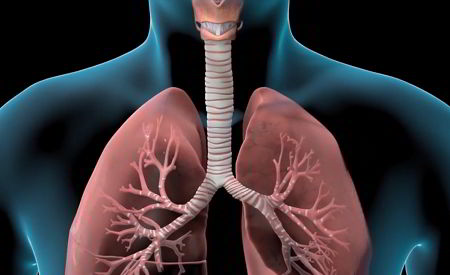
Every time we breathe, air passes down our windpipe (trachea), then into smaller passages called bronchi, then into even smaller passages called bronchioles, and finally into alveoli, which are the basic units required for respiration.
The alveoli are little air sacs that are surrounded by capillaries carrying blood. When we breathe in, the alveoli transfer oxygen (O2) from the lungs into the capillaries; when we breathe out, they transfer carbon dioxide (CO2) from the capillaries into the lungs.
The destruction of lung tissue alters the anatomy of the lung: the airways (bronchioles), which are surrounded by lung tissue, collapse and make breathing increasingly difficult. As a result the body does not get sufficient oxygen.
Three types of Emphysema can occur:
- Centriacinar Emphysema starts in the bronchioles and spreads mainly in the upper part of the lungs. It is generally associated with long-term cigarette smoking.
- Panacinar Emphysema is confined mainly to the bottom part of the lungs and destroys the alveolar tissue.
- Paraseptal Emphysema localizes around the septae of the lungs, which separate adjacent alveoli in the lung tissue. This can be caused by a history of lung infections.
Incidence; Causes and Development
Emphysema is more common in adult males than in females, and in those aged over 40 because lung function normally declines with age.
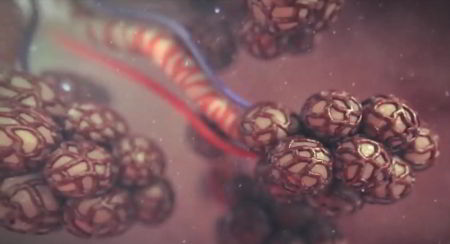
If a septum (the thin wall which separates the alveoli) becomes too stretched over time, several of the little sacs will join together, decreasing the surface area that is available for oxygen and carbon dioxide exchange. If enough of these sacs lose their separateness, like many small soap bubbles joining to make a few larger ones, breathing gets harder because each breath accomplishes less interchange of gases, resulting in Emphysema.
Caused by years of bad asthma, tobacco smoking, chemical damage, and other chronic lung disorders, it can be halted but not reversed. The first breath you take defines forever the number of the alveolar bubbles: they cannot be regenerated if they coalesce together.
Smoking cigarettes is by far the biggest contributor to Emphysema development – in fact at least 85% of all cases are caused by it. Some heavy smokers, however, will never develop Emphysema because they are not genetically susceptible to it.
Genetics comes into play when a person is born with deficiency of α1-Antitrypsin, which is a protein that protects the lungs from deteriorating. This deficiency can lead to the development of Emphysema at a relatively young age, even in non-smoking individuals.
Other possible causes of Emphysema include air pollution, inhalation of toxins or chemicals (including second-hand cigarette smoke), occupational dust from minerals, and the smoke from indoor heating or cooking.
Signs and Symptoms
Key symptoms of Emphysema are shortness of breath and a chronic cough. During the early stages of Emphysema development these symptoms might only be experienced during physical exertion. As the disease progresses, symptoms start to occur while at rest also.
Other symptoms can include:
- Frequent lung infections
- Mucus
- Weight loss and loss of appetite
- Fatigue
- Depression and anxiety
- Pale, gray or blue lips
Diagnosis and Tests
Pursed Lips Breathing, which is also a technique used to relieve symptoms, is one sign that might lead a doctor to suspect COPD/Emphysema.
Breathing tests can be used to confirm the presence of Emphysema: the patient takes a deep breath and then exhales as fast as possible into a machine that measures the airflow pressure. Those with Emphysema will experience a slower exhalation rate than normal due to the collapsed bronchioles in their lungs. Other breathing tests can measure diffusing capacity, which indicates the extent of damage to air sacs.
A chest X-ray can also be used to identify changes in the lungs that might be an indication of Emphysema, and detect any infections or masses in the lungs that could explain the symptoms.
A blood test is useful if the patient has a family history of α1-Antitrypsin deficiency. Blood tests can also be used to look at the white blood cell (WBC) count which might indicate an acute infection. This information, along with the chest X-ray, is used to diagnose pneumonia and bronchitis, which may be making Emphysema symptoms worse.
Treatment and Prevention
The first step in Emphysema treatment for smokers is to quit smoking. This will stop the progression of the disease but will not cure it; the rapid deterioration of the lungs will slow down to the normal rate that comes with age.
A doctor can prescribe bronchodilating medication that will cause the airways in the lungs to open wider (dilate) and allow better air exchange. The most common bronchodilator prescribed for Emphysema is albuterol (Proventil or Ventolin) because it provides fast relief for about 4 to 6 hours.
Albuterol can also be inhaled by using a nebulizer. The vaporized medication is released through a continuous air flow that is inhaled by the patient. This is often prescribed when the bronchodilator no longer alleviates shortness of breath.
Steroid medications are not effective with all patients but can sometimes be used to decrease inflammation in the lungs and relieve the symptoms of Emphysema.
In cases where the patient experiences an increase in shortness of breath, antibiotics may be prescribed even if chest X-rays show no indication of pneumonia or other infection. Antibiotics have been proven to decrease episodes of shortness of breath.
If a patient experiences severe shortness of breath and is hospitalized, oxygen is normally given. A plastic tube can be inserted into the patient's windpipe to allow machine-assisted breathing. Home-based oxygen tanks are also available that will allow a patient to perform normal day-to-day activities.
In patients with COPD (which can refer to Emphysema or Chronic Bronchitis), and those suffering from an asthma attack, the Pursed Lips Breathing (PLB) method is particularly useful for maintaining pressure within the airways and preventing the large airways from collapsing. It also promotes deep breathing, reduces shortness of breath, and is something that can be done any time, for example first thing in the morning, last thing at night, or when engaged in strenuous activity. The technique is simple:
- Breathe in normally
- Purse your lips as if blowing out a candle
- Breathe out slowly and gently through your pursed lips
Prognosis; Seek medical attention if...
Follow-up monitoring and care is very important in the management of Emphysema. Although there is no cure, progression of the disease can be slowed down to allow a relatively a normal life. Regular visits to the doctor and taking prescribed medication is essential.
If shortness in breath becomes increasingly worse, it is wise to seek medical attention. Signs of a serious lack of oxygen include the inability to speak full sentences, and the lips, tongue and fingernails turning a shade of blue.
On This Page
Emphysema:Signs, symptoms & indicators of Emphysema:
Symptoms - Environment
 Difficulty breathing in cold weather
Difficulty breathing in cold weather
Cold, dry air can cause narrowing of the airways in some people with chronic bronchitis or emphysema, which makes breathing more difficult.
 Breathing unaffected by cold weather
Breathing unaffected by cold weather
Cold, dry air can cause narrowing of the airways in some people with chronic bronchitis or emphysema, which makes breathing more difficult.
Symptoms - Nails
Risk factors for Emphysema:
Lab Values - Scans
 Normal chest X-ray or recently-normalized chest X-rays
Normal chest X-ray or recently-normalized chest X-rays
A chest X-ray may show changes caused by emphysema, including significant lung enlargement, scarring and hole formation.
Click to see sample report
Your body is a highly complex, interconnected system. Instead of guessing at what might be wrong, let us help you discover what is really going on inside your body based on the many clues it is giving.
Our multiple symptom checker provides in-depth health analysis by The Analyst™ with full explanations, recommendations and (optionally) doctors available for case review and answering your specific questions.
KEY